Mast cell tumors are the most common type of skin tumor found in dogs and the second most common skin tumor in cats. These represent 14–21% of all skin tumors diagnosed in dogs. They are usually noticed in middle aged patients, but can occur in patients of any age. Boxers and Boston terriers make up ~ 50% of all cases. Other common breeds affected include:
- Pugs
- Bullmastiffs
- Cocker spaniels
- Bull terriers
- Staffordshire terriers
- Fox terriers
- Labrador retrievers
- Golden retrievers
- Beagles
- Schnauzers
- Weimaraners
Most tumors are solitary although boxers and pugs have an increased predilection for multiple skin tumors. These tumors most often are noticed in the skin and subcutaneous tissue. Common locations in the dog include:
- Trunk 42–65%
- Limbs 22–43%
- Head and neck 10–14%
Visceral (intra-abdominal organs) mast cell disease is a recognized form of the disease and is more aggressive than the aforementioned locations. This is often preceded by skin or subcutaneous tumors.
Your pet’s clinical signs will relate to the grade and progression of the disease. Some pets will be presented with small, freely movable tumors in the skin or subcutaneous tissues with minimal surrounding inflammation. Other pets will be presented with large, ulcerated, and hairless tumors often associated with a more aggressive tumor. Clinical signs such as vomiting, loss of appetite, and digested blood present in the stool are also possible. The grade and subsequent prognosis related to the tumor cannot be determined until it is removed and submitted to histopathology for analysis biopsy and histopathologic analysis has been performed.
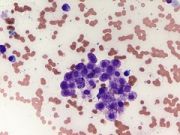
Mast cell tumors can vary in size from day to day, depending on the degree of inflammation secondary to the degranulation of the cells. This occurs when the small dark staining granules inside the cells (Figure 1) are released and irritate the adjacent tissues. These granules contain histamine, proteolytic enzymes (denature proteins), and vasodilatory substances responsible for the redness and swelling surrounding your pet’s tumor. These same factors can also effect the gastrointestinal tract causing ulcers resulting in clinical signs such as vomiting, lack of appetite, melena (bloody stool), anemia (low red blood cells), and abdominal pain.
Mast cell tumors can be accurately diagnosed with a simple needle aspirate of the tumor in almost all cases. These cells show characteristic dark blue to purple intracellular granules (Figure 1). As discussed earlier, these granules contain inflammatory substances that contribute to the clinical signs your pet may exhibit. Some mast cell tumors do not have dark staining granules and these necessitate advanced cytologic evaluation such as immunohistochemistry at the time of histopathologic evaluation. The grade of the tumor which determines the overall prognosis for your pet can only be evaluated after a surgical biopsy and histopathologic analysis of the tumor has been performed. The tumor is removed and submitted for histopathology.
Metastasis (spread of tumor cells) occurs first at the local lymph nodes and then potentially to the bone marrow and visceral organs such as the spleen, liver, lungs (rarely), and other regions of the skin. As such, your pet’s primary care veterinarian or ACVS board-certified veterinary surgeon may recommend additional staging tests for your pet to look for evidence of metastasis at the time of diagnosis. This may include a needle aspirate of the regional lymph nodes or abdominal organs to look for evidence of metastasis at the time of diagnosis. Furthermore, staging of animals with cancer often may include an abdominal ultrasound and/or chest x-rays to determine if there is evidence of malignant cancerous cells. Abdominal ultrasound is used to evaluate the gross size, shape, and texture of abdominal organs. Chest x-rays may also be recommended to rule out concurrent cancers or diseases that may affect your pet’s long term prognosis prior to surgical recommendations.
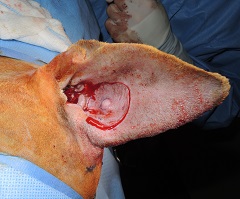
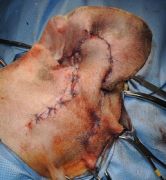
Surgical removal of mast cell tumors is the preferred treatment once your pet is diagnosed with this disease. Mast cell tumors invade into surrounding tissues and wide surgical margins (wide area of healthy tissue surrounding the tumor Figure 2 and Figure 3) are necessary to ensure removal of all cancerous cells. The excised (removed) tumor will be submitted for histopathology for confirmation of the tumor type and grading. Prior to surgery your pet’s primary care veterinarian or veterinary surgeon may recommend medical management. This often may includes steroids, anti-histamines, and histamine blockers to help reduce the inflammation and associated side effects of these tumors prior to surgery.
Post-surgical radiation and chemotherapy are warranted on a case-by-case basis. Radiation is most commonly used as a multi-modal treatment approach for incompletely excised tumors. Chemotherapy is used in patients with disseminated disease to other organs or high grade tumors. Your pet’s primary care veterinarian and veterinary surgeon will work together to make the most appropriate recommendation for your pet’s continued care following surgery.
Boxers and pugs are more likely to have low grade tumors than other breeds. The grade of the tumor directly relates to the prognosis for your pet. The grade cannot be determined until it is removed surgically and evaluated using histopathology. This includes looking at a sample of the tumor under a microscope. Tumor grade is based on the invasion of the tumor into surrounding skin and other tissues, the number of actively dividing cells, abnormal cellular morphology, and the characteristics of the intracellular structures. The grade will dictate the metastatic potential (chance of tumor spread), long-term survival time, and necessary follow-up treatment options such as chemotherapy. Generally speaking, lower grade tumors have longer survival times and higher grade tumors have shorter survival times. Additional prognostic factors include breed, clinical presentation, tumor location, staging results, and surgical margins. Your pet’s ACVS board-certified surgeon will discuss these results with you to develop a specific treatment plan for your pet following surgery.
Genetic analysis of the tumor may also be recommended by your pet’s ACVS board-certified veterinary surgeon. This test is used to look for a certain cellular growth factor called KIT (CD117) or more commonly known as the C-Kit Mutation. The C-Kit mutation is an abnormality with a specific cellular receptor involved with proliferation and other biologic activities. This mutation is more common with higher grade tumors resulting in higher recurrence rates, increased cellular proliferation, and ultimately shorter survival times. This mutation is present in approximately 15–40% of mast cell tumors.
Feline Mast Cell Disease:
Feline mast cell disease is different from mast cell tumors found in canine patients. It accounts for 8-21% of skin tumors in cats. The most common feline breed associated with this disease is the Siamese cat. Unlike the dog, the most common locations found in feline patients are the head and neck followed by the extremities. Additionally, cutaneous mast cell tumors found on the head and neck of cats are less aggressive than those found in dogs. Some cutaneous mast cell tumors will spontaneously regress. However, if you notice a tumor on your cat it is recommended to schedule an appointment with your primary care veterinarian for evaluation. Cats with cutaneous mast cells still need clinical staging prior to surgery to evaluate for metastasis. The overall prognosis for cats with the cutaneous form of this disease is good with low recurrence rates. A more serious form of mast cell tumors exists in cats known as the visceral form where the intestines or spleen is affected without any tumors on the skin. Removal of the spleen should be pursued in these cases. This form carries a poor prognosis and is associated with clinical signs such as vomiting, weight loss, and loss of appetite.