Perineal hernias result from weakening or complete failure of the muscular diaphragm of the pelvis. There are multiple muscles that make up the pelvic diaphragm, which work together for rectal support and keeps the abdominal contents from encroaching the ischiorectal fossa. The most common perineal hernia occurs between the levator ani, internal obturator and external anal sphincter and is termed a caudal perineal hernia. Other perineal hernias include the dorsolateral (between the coccygeus and levator ani), ventral (between the ischiourethralis, bulbocavernosus, and ischiocavernosus muscles) and sciatic perineal hernia (between the coccygeus and sacrotuberous ligament), Combinations of these hernias can also occur on the same side or also on the opposite (contralateral) side. As a result of this weakness, retroperitoneal fat, omentum, or abdominal organs can herniate in the ischiorectal fossa, resulting in a visible perineal protrusion. Pets with perineal hernias can demonstrate a swelling adjacent to the rectum on one or both sides coupled with signs of constipation, difficulty defecating, lethargy, difficulty urinating, and altered tail carriage.
The disease primarily affects older pets, usually between the ages of 7 to 9 years. The exact underlying cause for weakening or failure of the pelvic diaphragm is unclear at this time. However, many theories are proposed, all of which may be working separately or in unison to allow for pelvic diaphragm weakening or failure. Because non-castrated male dogs and cats are predisposed to this condition and castration at the time of hernia repair seems to reduce the incidence of recurrence, the presence of androgens seems to be an important contributing factor to the cause of this condition. Other factors may include structural weakness of the pelvic diaphragm, neurologic damage to the nerves that innervate the pelvic musculature or concurrent abdominal disease that lead to straining.
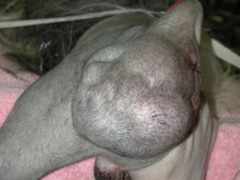
Pets with perineal hernias typically demonstrate a swelling adjacent to the anus on one or both sides (Figure 1). The swelling may contain herniated abdominal and pelvic canal contents, such as retroperitoneal fat, omentum, dilated rectum, prostate, urinary bladder, and small intestine. Clinical signs seen in pets with perineal hernias are related to the organs entrapped in the hernia. Typically, these signs include:
- constipation
- straining to defecate
- straining to urinate
- inability to urinate
- urinary incontinence
- abdominal pain
- lethargy
- depression
- anorexia
- altered tail carriage
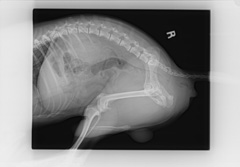
To diagnose perineal hernia your veterinarian will perform a thorough rectal examination. This will help to determine the presence or absence of a mass-like lesion, prostate disease, contents of the hernia, and to determine unilateral or bilateral disease. Some pets may require analgesic or sedative administration for completion of a rectal exam. Once the diagnosis of perineal hernia has been made, a thorough metabolic and abdominal work-up should be instituted. Your primary care veterinarian will likely recommend a complete blood count, biochemical profile, and urinalysis to determine any concurrent systemic illness. Advanced diagnostic imaging (ultrasound and abdominal radiographs) may be recommended to help determine hernia contents, bladder position and size, colon position and size, prostate disease, or the presence of cancer (Figure 2).
Pets demonstrating any swelling adjacent to the rectum along with the clinical signs mentioned above should seek veterinary advice as soon as possible. Organ entrapment into the perineal hernia may be life threatening and necessitate emergency stabilization prior to definitive surgical intervention. Your veterinarian may wish to refer you and your pet to an ACVS board certified veterinary surgeon for surgical repair of a perineal hernia.
Perineal hernias, by themselves, may cause constipation, which in turn, may damage the motility function of the colon. Perineal hernias may also disrupt your pet’s ability to urinate. Occasionally excessive straining may cause the urinary bladder to retroflex (flip over backwards into the pelvic canal) leading to urinary obstruction and potentially loss of blood supply to the bladder. Entrapment of a loop of intestine into the hernia may cause significant pain and loss of the blood supply. Emergency surgery is indicated for pets with signs of abdominal pain, inability to urinate, and a strangulated loop of small intestine.
Treatment of non-emergency perineal hernia may consist of either medical or elective surgical therapy. Medical therapy is indicated for preparing a pet for surgery, but is generally unsuccessful at permanently controlling the disease process. Medical management will consist of a combination of enemas, stool softeners, IV fluid therapy, dietary management, and analgesics.
Surgery is aimed at repairing the pelvic diaphragm and preventing recurrence. A perineal herniorrhaphy typically involves placing sutures to anatomically restore the pelvic diaphragm. The incorporation of a muscle flap may help to bolster this repair. The internal obturator is a muscle along the floor of the pelvis and is the most common one to be used as a flap. Other surrounding muscles, such as the superficial gluteal or semitendinosus muscles, can also be used for severe cases. Surgical mesh may also be implanted in cases where a defect persists despite anatomic and muscle flap reconstruction. Recent studies have also indicated that many pets that present with unilateral perineal hernia may also have a subtle perineal hernia on the opposite side. Your surgeon may recommend surgery on the contralateral side as well.
Additional surgical treatment may include performing an organopexy, which involves placing suture to permanently anchor an organ to the adjacent abdominal wall. This can diminish the likelihood that the organ would retroflex into ischiorectal fossa. This procedure can be performed on the colon (colopexy), bladder (cystopexy), and/or vas deferens (vas deferensopexy). Organopexies should be considered in cases where these organs have already herniated into the ischiorectal fossa or for pets that have recurrent perineal hernias.
It is recommended that all pets be castrated during the surgical procedure to help decrease the risk of reoccurrence.
During initial hospitalization, all pets are monitored for complications. Many complications are considered minor complications and do not require a second procedure. These minor complications may include surgical site infection due to the close proximity of incision to the anus, wound dehiscence, bruising, transient discomfort during defecation, urgency to defecate without producing any stool, and swelling around the surgical site. With time and the appropriate medical treatment, these clinical signs should resolve in a few days to weeks. Other complications can include fecal incontinence or urinary tract issues, especially if the bladder had been entrapped.
Complications that may require a revision procedure would include instances of nerve entrapment or hernia recurrence. Nerve entrapment is typically noted immediately after surgery since these pets are noted to be significantly painful postoperatively and may have weakness or deficits associated with the hindlimb. Recurrence of a perineal hernia can occur despite robust surgical technique. Recurrence rates can range from 10-50% depending on the surgical methods used to address the defect.
In uncomplicated cases, the typical post-operative recovery timeframe is around 2 weeks. If complications are noted, your surgeon will discuss with you the appropriate intervention.